Reactive oxygen species, or ROS, are unstable molecules produced during mitochondrial metabolism. These molecules can cause a host of problems, attacking brain tissue and causing oxidative damage. Now, a group of scientists has found a link between ROS and Alzheimer’s disease (AD), demonstrating that AD progression is closely associated with oxidative brain damage caused by ROS. Read on to find out how the researchers used a 5xFAD transgenic mouse model to make this connection.
Building on a Previous AD Breakthrough
In a 2016 study, a team of scientists used rat models to explore oxidation levels in test animals with vitamin E deficiency. The researchers found that oxidation levels were substantially higher in older rats with vitamin E deficiency than in younger rats. At the same time, it became clear that high oxidation levels could have a negative effect on brain cells. The researchers felt that this implied a link between AD, which is a condition linked to oxidative stress, and ROS produced due to mitochondrial oxidation dysfunction – but they needed to explore further. Now, that same team of researchers has confirmed that the progression of AD is closely associated with mitochondrial oxidation dysfunction and, thus, oxidative brain damage. That study, led by Professor Koji Fukui, along with his colleagues Naoki Yoshida, Yugo Kato, and Professor Hirokatsu Takatsu, was recently published in Biomedicines.
Studying 5xFAD Transgenic Mouse Models
For the most recent study, the scientists used three groups of 5xFAD transgenic mice aged three, six, and 20 months. They compared these mice to a set of healthy control mice. The researchers began by testing the animals’ cognitive abilities and coordination, which involved two standard experiments: the Morris water maze and the RotaRod test. In the water maze test, 5xFAD transgenic mice took longer to complete the maze but did not slow down. Interestingly, in the RotaRod test, the six-month-old and 20-month-old 5xFAD mice stayed on the rod for a longer time than the age-matched control mice. According to study lead Koji Fukui, that could be attributed to the weight difference between the two groups; the control mice were heavier than the 5xFAD mice. Ultimately, the results suggested that the 5xFAD mice may have been cognitively impaired, but did not experience coordination problems.
Assessing Cognitive Impairment in 5xFAD Transgenic Mouse Models
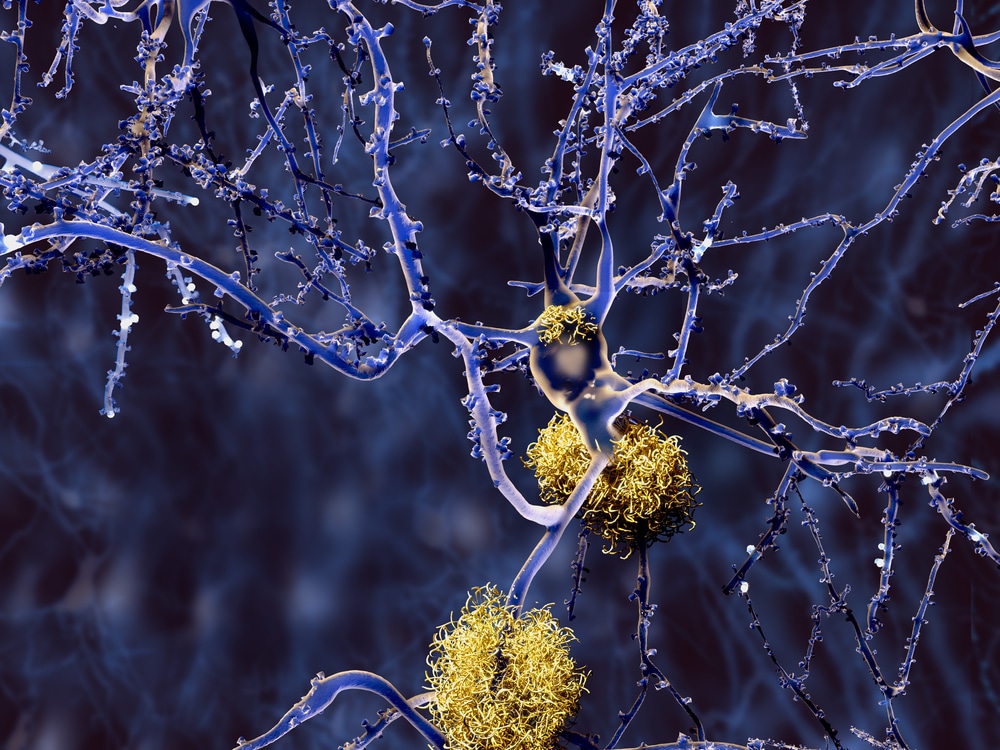
The team confirmed that the 5xFAD mice experienced cognitive impairment. However, they were unsure which AD-related proteins were responsible for the phenomenon. To find out, the researchers collected tissue samples from various parts of the brain from both groups of mice. The team then assessed the oxidative markers in each sample. Their findings were fascinating. First, they found that 5xFAD mice had higher levels of Aβ, the protein associated with the progression of AD. The 5xFAD mice also showed a gradual increase of Aβ with age. Also interesting was the fact that the AD-related protein Aβ1-42 was much higher in the hippocampus than in other parts of the brain. Overall, the team was able to confirm that Aβ1-42 aggregation in the hippocampus directly caused cognitive impairment in the test subjects.
Mitochondrial Damage and Neuron Survival
Finally, the team related their findings back to ROS. They initially hypothesized that ROS-induced mitochondrial damage was closely related to brain neuron death seen in AD patients. The researchers explored this hypothesis by checking the levels of key mitochondrial oxidative enzymes in the 5xFAD mice. One of those enzymes, 3-NT (3-nitrotyrosine), is an indicator of higher oxidation – and was found to increase with age in the 5xFAD mice. This was proof that oxidation causes mitochondrial dysfunction, eventually leading to the cognitive dysfunction seen in AD progression.
_____
By studying 5xFAD mice, Professor Fukui’s research team was able to identify a key connection between oxidation, mitochondrial dysfunction, and AD progression. With this in mind, the team may be able to make other connections that will advance the treatment of this devastating disease.
Scantox is a part of Scantox, a GLP/GCP-compliant contract research organization (CRO) delivering the highest grade of Discovery, Regulatory Toxicology and CMC/Analytical services since 1977. Scantox focuses on preclinical studies related to central nervous system (CNS) diseases, rare diseases, and mental disorders. With highly predictive disease models available on site and unparalleled preclinical experience, Scantox can handle most CNS drug development needs for biopharmaceutical companies of all sizes. For more information about Scantox, visit www.scantox.com.
