Experimental autoimmune encephalomyelitis (EAE) shows many pathological similarities to Multiple Sclerosis (MS) and is therefore often used as model to mimic MS by injecting Myelin-Oligodendrocyte-Glycoprotein (MOG) in combination with pertussis toxin (PTX).
C57Bl/6 mice develop clinical signs about two weeks after MOG + PTX treatment. Fingolimod (Fingo) was able to reduce clinical signs reaching significance after 2 weeks of treatment (Fig. 1a). Evaluation of all animals in the Open Field test showed that MOG + PTX treatment resulted in a completely diminished rearing behavior. Fingolimod was not able to rescue this phenotype (Fig.1b). Analysis of muscle strength in the Wire suspension test showed a severely reduced hanging time of MOG + PTX treated mice. This phenotype could be partially rescued by Fingolimod (Fig.1c). Motor coordination of MOG + PTX treated animals was thus also strongly impaired as analyzed in the RotaRod test. Fingolimod was also able to partially rescue this phenotype (Fig.1d).
MOG + PTX treated mice closely mimic EAE symptoms and are therefore a good model for Multiple Sclerosis. The model is widely used as primary screening tool for new MS compounds.
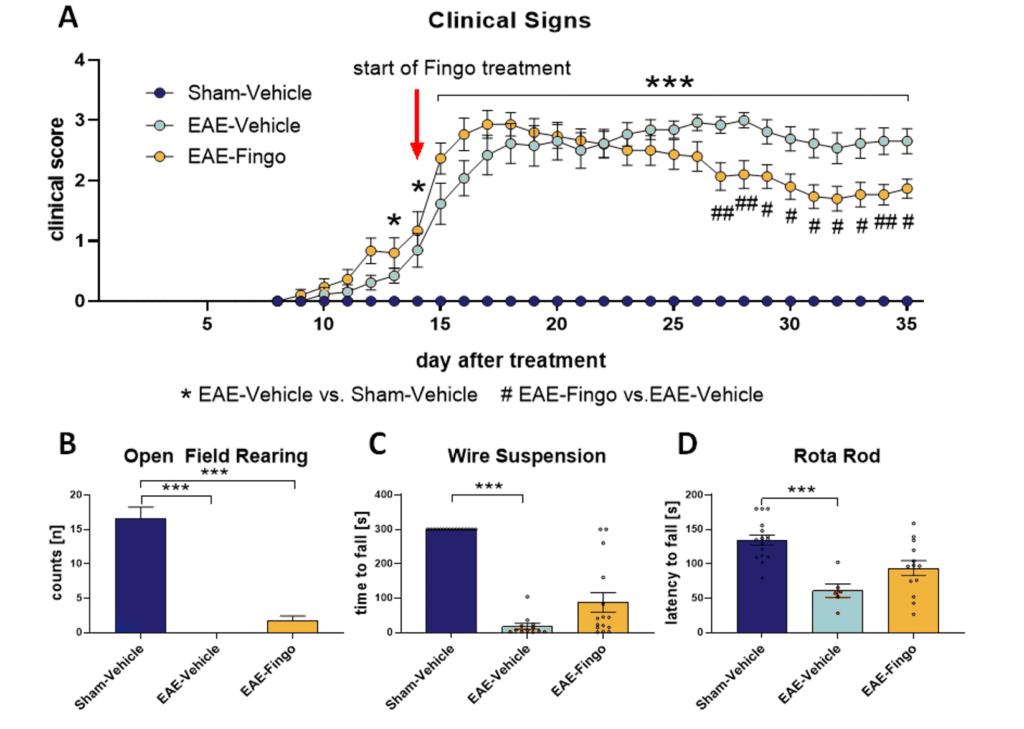
Figure 1: Clinical signs and motor deficits of EAE mice. EAE induced C57Bl/6 mice were tested for clinical signs (A), rearing activity in the Open Field test (B), muscle strength in the Wire suspension test (C) and motor coordination in the RotaRod test (D) compared to vehicle treated and EAE + Fingo treated mice. n = 13-16 per group; Mean + SEM; Kruskal-Wallis One-way ANOVA followed by Dunn‘s multiple comparisons post hoc test; *p<0.05; **p<0.01; ***p<0.001. *EAE-Vehicle vs. Sham-Vehicle; #EAE-Fingo vs. EAE-Vehicle. Fingo = Fingolimod.
